Where should we donate to do the most good? - Essay Competition Winner
This is the winning essay in our competition.
Where should we donate to do the most good?' What is the most effective, scalable, evidence-based, but currently underfunded global health intervention that is already being implemented or could be implemented soon?
Most development failures happen at delivery.
In 2004, a World Bank report stated that deaths from malaria could be “all but eliminated” using then available treatment interventions (World Bank, 2004). But ten years later, malaria still kills over 500,000 people every year (World Health Organization, 2014).
One estimate suggested that if use of all the proven effective childhood preventive and treatment interventions were to rise from current levels to 99 % (95% for breastfeeding), the number of under-five deaths worldwide could fall by 63% (Jones, Steketee, Black, Bhutta, & Morris, 2003).
We invest billions of dollars in finding the next vaccine, the next drug, the next possible intervention. But not nearly so much in improving the delivery of interventions we already know work well. These are primarily not scientific or technological challenges. They are challenges of implementation, of delivery.
So what is an example of a delivery intervention we should be trying?
Alma Sana Inc. is a social enterprise founded in 2012. Its key innovation is to use simple vaccine reminder bracelets which are worn by children from birth to age four years old.
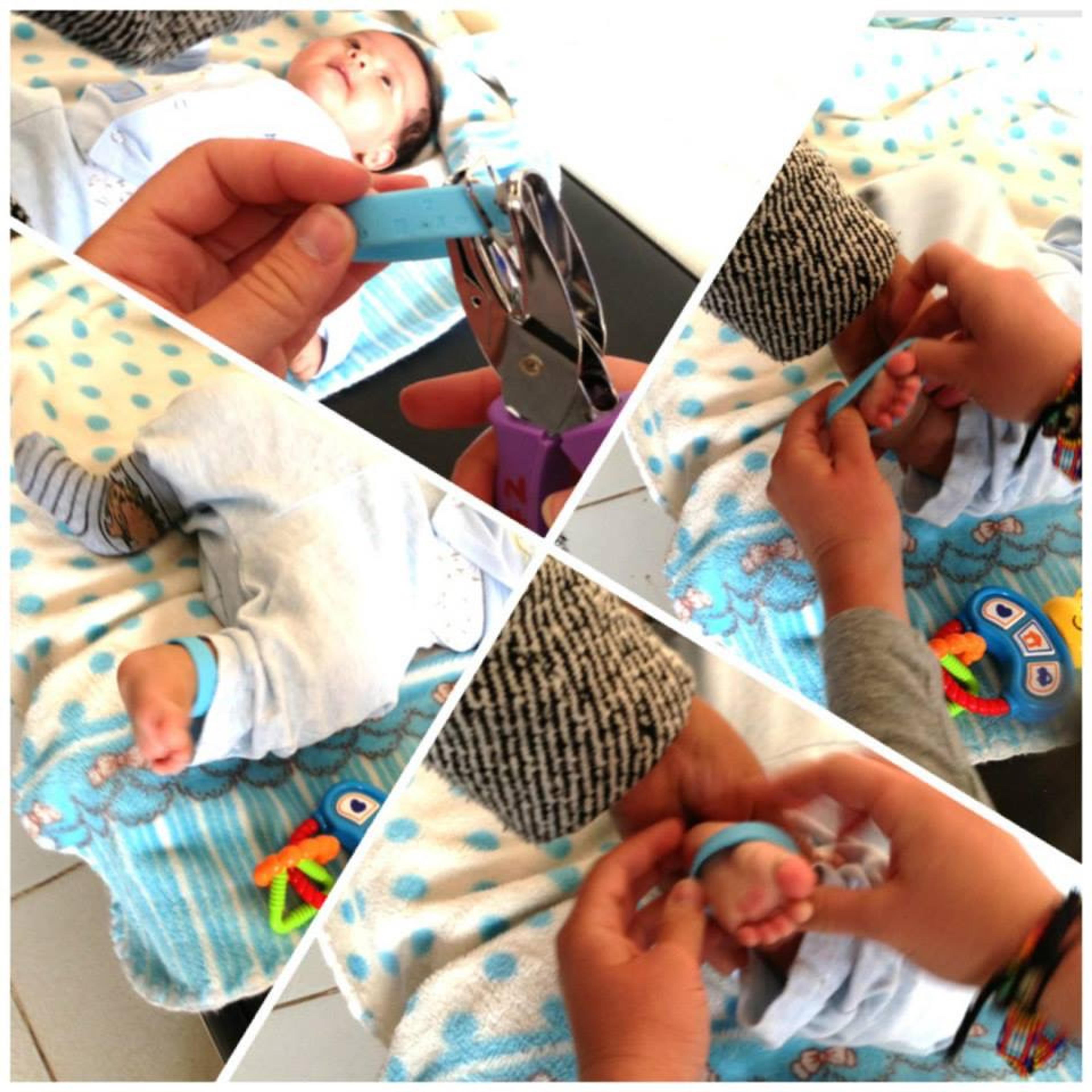
Vaccines are highly effective, scalable and have one of the best evidence bases of any intervention in health (according to GiveWell and the Copenhagen Consensus). The number one risk factor in infectious disease is failure to vaccinate (McHugh, Guarecuco, Langer, & Jaklenec, 2015). Yet an estimated one in five children in the world do not receive full or timely immunisation. Vaccines are one of our best weapons against poverty and ill health, yet we aren’t getting them to over 18 million children.
Failure to provide reminders and the forgetfulness of caregivers are key reasons for missed vaccinations across a wide range of contexts (Patel & Pandit, 2011)(Wakadha et al., 2013)(Wilson, 2000)(Quaiyum et al., 2011). Mothers may be illiterate and struggle to understand routine immunisation cards.
The Alma Sana bracelet is worn by the child and uses symbols for each disease which are ‘punched out’ when a vaccine has been delivered. The bracelet has been implemented in an initial 6 month pilot study in rural Peru and Ecuador. A bracelet costs $0.10 to produce. Initial results are positive. 91% of mothers said the bracelets helped remind them of vaccination visits. 90% said they would continue to use the bracelets in the future if possible. 87% said they would recommend the bracelets to other mothers. The next step of the innovation is to run a larger 1 year study with 5,000 mothers and babies. Further information is at the Alma Sana website.
Could this be a viable, practical solution for the challenge of vaccine delivery? Perhaps. We need to test it. Adapt it. Iterate. But this is the sort of innovation needed to get to the 20% of unvaccinated children who are hard to reach.
In Bangladesh, relatively simple innovations such as adding the phone number of vaccinators to immunisation cards helped increase immunisation coverage by 15% in a single year (Save the Children, 2012). Bangladesh is one of the poorest countries in the world but its national immunisation coverage rate (measured using DPT3 rate) is 95% (WHO & UNICEF, 2014). This should be achievable for all countries if the right focus is placed on delivery and experimentation.
The beauty of this Alma Sana vaccine bracelet is that it has the potential to improve service delivery of all childhood vaccinations- an enormous potential impact at a very low cost. Vaccinations are already seen as a ‘best buy’ in public health and highly cost-effective (World Health Organization, UNICEF, & World Bank, 2009).
When considering whether to fund an innovation, we should think about both the impact it could have and the likelihood of achieving that impact. At this stage we cannot say for certain whether the vaccine bracelets will be effective at increasing immunisation rates despite early positive indications. But for approximately $1m this intervention will be rigorously trialled in three different countries to establish whether it works. Given the very low intervention cost even a small improvement in vaccination rates is highly likely to be cost-effective.
Giving What We Can rightly has a focus on what areas are underfunded. As an organisation that can only realistically hope to direct or steer a minority of philanthropic donations this is an absolutely appropriate goal. But Giving What We Can should also consider its comparative advantage when compared to other funding organisations.
Facing a choice between donating to two equally effective organisations, GWWC donors should choose the more obscure, the smaller, less well-known alternative. They are less likely to get the money some other way. Alma Sana is a small social enterprise that has to date received a small grant from the Gates Foundation and some money from a crowdfunding campaign. I do not know their internal financial picture, but it seems unlikely that they currently have the money to fund worldwide trials and they certainly do not have the resources to scale this intervention nationally should it prove successful.
This is where Giving What We Can donors should put their money. Not in the ‘sexy’ development of new drugs, or in the already well-funded, tried and tested rollout of malaria bednets. But in the vital, dull yet risky work of optimising the delivery of proven interventions to make sure they reach everyone who needs them. Alma Sana is an excellent example of the sort of service delivery innovation that is so badly needed.
Bibliography
- Jones, G., Steketee, R. W., Black, R. E., Bhutta, Z. A., & Morris, S. S. (2003). How many child deaths can we prevent this year? Lancet (London, England), 362(9377), 65–71.
- McHugh, K. J., Guarecuco, R., Langer, R., & Jaklenec, A. (2015). Single-injection vaccines: Progress, challenges, and opportunities. Journal of Controlled Release : Official Journal of the Controlled Release Society.
- Patel, T. A., & Pandit, N. B. (2011). Why infants miss vaccination during routine immunization sessions? Study in a rural area of Anand District, Gujarat. Indian Journal of Public Health, 55(4), 321–3.
- Quaiyum, M. A., Gazi, R., Khan, A. I., Uddin, J., Islam, M., Ahmed, F., & Saha, N. C. (2011). Programmatic aspects of dropouts in child vaccination in Bangladesh: findings from a prospective study. Asia-Pacific Journal of Public Health / Asia-Pacific Academic Consortium for Public Health, 23(2), 141–50.
- Save the Children. (2012). Immunisation for All: No Child Left Behind.
- Wakadha, H., Chandir, S., Were, E. V., Rubin, A., Obor, D., Levine, O. S., … Feikin, D. R. (2013). The feasibility of using mobile-phone based SMS reminders and conditional cash transfers to improve timely immunization in rural Kenya. Vaccine, 31(6), 987–93.
- WHO, & UNICEF. (2014). Bangladesh: WHO and UNICEF estimates of immunisation coverage: 2014 revision. Retrieved August 31, 2015, from http://www.who.int/immunization/monitoring_surveillance/data/bgd.pdfWilson, T. (2000). Factors influencing the immunization status of children in a rural setting. Journal of Pediatric Health Care : Official Publication of National Association of Pediatric Nurse Associates & Practitioners, 14(3), 117–21.
- World Bank. (2004). The Millennium Development Goals for Health: Rising to the Challenges.
- World Health Organization. (2014). WORLD MALARIA REPORT 2014 SUMMARY.
- World Health Organization, UNICEF, & World Bank. (2009). State of the world’s vaccines and immunisation.