For more information on this topic, see our section on emergency aid
Whenever a disaster happens, whether it’s an earthquake, a tsunami, or some new human conflict, we all feel that urge to reach into our pockets and give a little to help. We know that, in an emergency, there is a huge amount of suffering, whether that is through deaths, injuries or loss of property and livelihoods. And we think that, when someone has nothing, every little will help. And so we donate, knowing that when the worst comes, victims of a disaster will need all the help they can get. But is emergency aid really that effective? Should we instead hold ourselves back, and give to one of the recommended charities instead?

In 2006, the Disease Control Priorities Project released a damning report of humanitarian interventions in natural disasters, saying that “the highly emotional and sensationalized climate of disaster response has long prevented the adoption of a cost-effectiveness approach in decision making.”[1] The need for rapid response times and improvisation means that it is difficult to ensure cost-effectiveness. Even worse, the international community spends millions on short-term responses to disasters, but there is often not enough funding to ensure even the mid-term survival of victims. And the prevalence of coordination and congestion problems, as well as situations that are outside charities’ control, means that the success of response operations are often limited by factors other than funding, so that there is often very little room for more funding for emergency responses.
A look at Haiti[2]
On 12th January 2010, a magnitude 7.0 earthquake shook Haiti. The epicentre of the earthquake was just 17km from Haiti’s capital and largest city, Port-au-Prince, with a population of approximately 2 million. A huge number of buildings collapsed, including hospitals and other critical infrastructure. The drinking water and sewer systems were almost completely destroyed.[3]
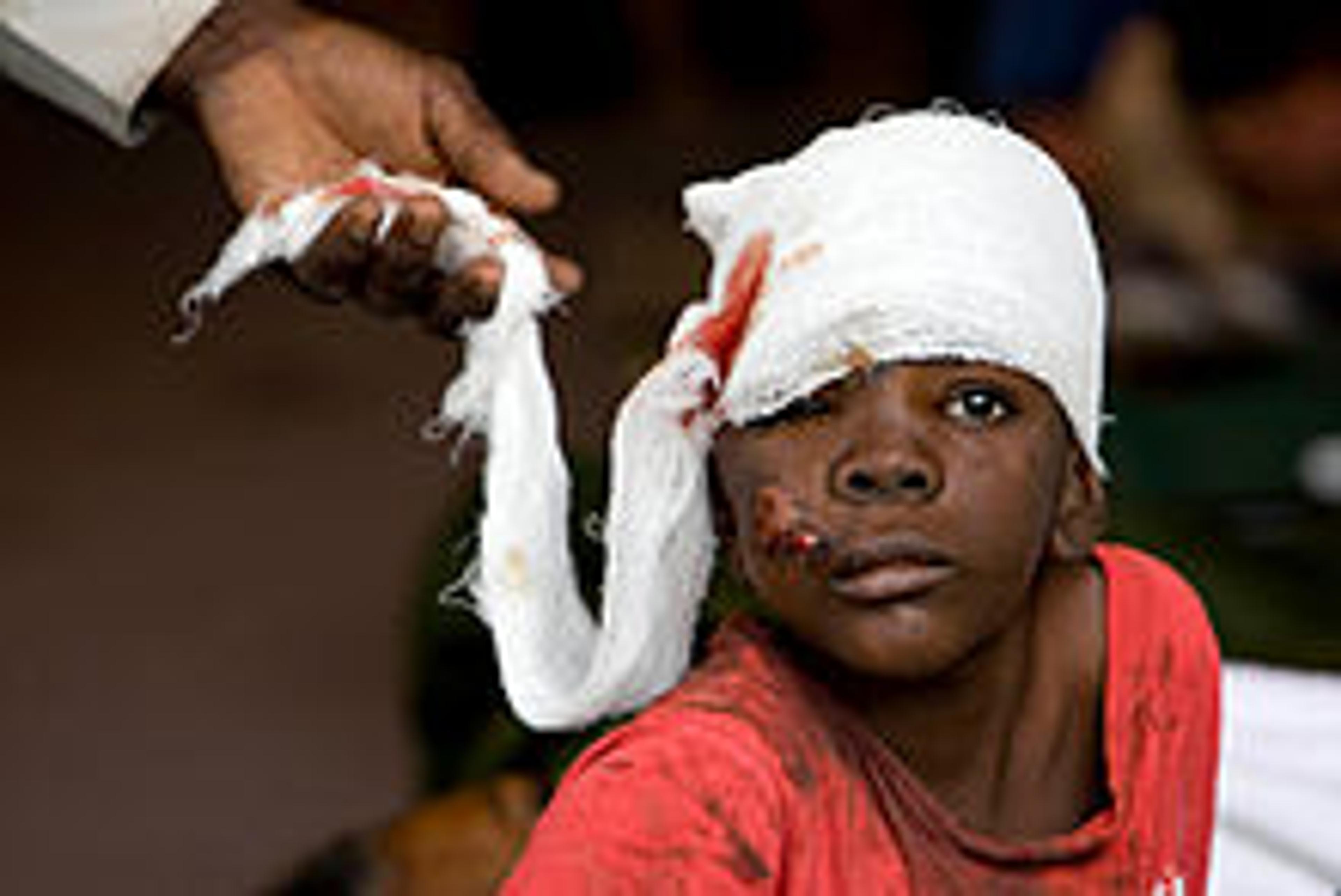
After the earthquake, there were an estimated 250,000 injured victims suffering a wide range of injuries. In the first few hours, first-aid and triage stations were vital. Within a few days, operations such as wound debridement and amputations were needed. And in the following weeks, surgical needs actually increased as more patients (often with infected wounds) sought medical care. In the weeks to months after the earthquake, non-trauma surgical needs such as maternity services increasingly needed to be provided by NGOs as the pre-earthquake health system collapsed.
The earthquake in Haiti produced a huge humanitarian response. However, the NGOs involved experienced a huge range of different problems that reduced the effectiveness of their operations. Notably, there were supply delays, a lack of appropriately experienced health professionals, and challenges in coordinating between government, military and non-governmental organisations.
Very few of the over 600 health agencies who responded to the Haiti earthquake had the relevant experience or competence to provide appropriate surgical care, and they often lacked the capacity to build emergency surgical infrastructure. A lack of coordination led to too many agencies trying to provide the same care in the same area, while other sections of Port-au-Prince (Haiti’s capital and largest and worst affected city) were left with no access to emergency care. After a few weeks, many military and humanitarian groups left, leaving behind thousands of post-operative patients. The lack of referral systems or any good communication between NGOs caused problems when patients stopped going to hospitals from groups that had left and moved to other NGOs’ hospitals.
Experienced agencies often have a shortlist of hotspot regions (such as central Africa for conflicts or central America for natural disasters). They then preposition materials at major airfields so that their proximity ensures a rapid response. However, prepositioning requires substantial maintenance costs and a high risk of waste as medical and food supplies expire. What’s more, proximity does not necessarily reduce response times. In the case of Haiti, airport congestion led to large delays getting through the medical equipment that was urgently needed to treat the quarter of a million injured victims of the earthquake. The US military-controlled Port-au-Prince airport gave dignitaries and high-profile media priority, while planes carrying humanitarian supplies were diverted to Santo Domingo (the capital of the neighbouring Dominican Republic), and transported the 200 miles to Port-au-Prince by land.
Finally, specialists (surgeons, anaesthesiologists, traumatologists, emergency medicine doctors) who are experienced in treating war-wounded as well as working in resource-limited settings are very rare. Inexperience in emergency settings can be a hindrance rather than a help. The American College of Surgeons listed hundreds of surgeons to go to Haiti, but agencies did not accept their help due to their inexperience.
These problems are indicative of issues encountered in the majority of emergency aid efforts. For example, poor coordination was criticised in response to the Rwandan genocide[4] and the 2004 Indian Ocean tsunami[5]. In the case of emergency aid it is also quite likely that uncontrollable (from an NGO’s perspective) events will occur that significantly hinder the response - in the case of Haiti it was the airport congestion, but in other cases it could be military blockades or overcrowding. Financial aid would not help in these situations, reducing the room for more funding for aid organisations.
Some specific interventions[6]
- Search and rescue teams are needed in the first 48 hours following a disaster involving the collapse of buildings. Very few developing countries have the expertise to conduct search and rescue missions in collapsed multi-storey buildings, so they are often sent at high cost from industrial nations. However, if not executed immediately, the value of search and rescue drastically decreases, as people who are trapped die quickly without treatment. As it also takes a long time for teams from other nations to reach the disaster zone, the large amount of money this requires is very inefficiently spent. Investing in local search and rescue teams is most likely to be an effective use of resources.
- Field hospitals are a common but very expensive way of treating casualties. They often arrive too late to treat the emergency casualties before they die or are treated by local hospitals. Field hospitals that stay longer than the first two to three weeks can be effective, although there is little data to suggest how effective compared with how local services would have taken immediate action. In the 2003 Bam earthquake, around $10.5 million was spent on about 10 mobile hospitals, but the cost of rebuilding the entire health infrastructure in the area was only $10.75 million!
- Preventing and controlling the spread of disease can be effective if effective methods (such as the use of insecticide-treated malaria nets or encouraging hand-washing with soap) are used. Another way of increasing the cost-effectiveness is by strengthening already-existing programs rather than starting new ones.
- Creating shelters is an important method of ensuring survival. However, tent cities, being easy to set up, are the most common method of doing this. Tent cities are difficult to sustain and nearly impossible to end. They rarely have effective sanitation and living conditions are poor. Distributing construction material or cash subsidies is more cost-effective, as they have greater positive effects in the long-term.
- Cash assistance is a plausibly effective method to aid with long-term recovery of a disaster. It cannot really be used to meet immediate life saving needs. in most disaster-affected countries, those with the largest income will more easily gain access to the services and goods they need, whether that be shelter, medical, food, or anything else. This suggests that income availability is often a limiting factor in long-term recovery, and that therefore cash assistance could speed up this recovery.
- Donating in-kind, for example by sending clothing or tinned food, whether to NGOs or from NGOs to countries, is of limited use, and, according to the Disease Control Priorities report, “often cause serious logistic, economic, and political problems in the recipient country”. They can divert humanitarian funds from more effective uses to warehousing supplies and building facilities for the safe disposal of pharmaceutical donations.
So is it actually overfunded?
In 2004, the Indian Ocean earthquake and tsunami sparked a huge number of donations, with 81% of UK adults donating to the campaign, and a total of £392 million being donated.[7] 25% of personal overseas charitable donations in 2004/2005 were to the tsunami appeal, and 20% of those were diverted from other causes.[8] If we assume that these donations would have also been on overseas aid, 5% of the total personal donations budget on overseas aid from the UK was diverted away from other causes to the already over-funded tsunami appeal. In 2010, 48% of UK adults donated to the Haiti earthquake appeal, with a total of £107 million donated:[9] 5% of overseas aid donations the Haiti appeal. Almost all major organisations, including the Red Cross, Médecins Sans Frontières, Oxfam, Save the Children and UNICEF raised significantly more than they spent in the first year after the earthquake, indicating the vast overspend and a lack of room for more funding in the Haiti appeal.[10]
With smaller events, the numbers are less staggering, though still surprising. With the 2008 Burma Cyclone, 23% of UK adults donated a total of £19.5m, and in the 2009 Asia-Pacific disasters, 23% of UK adults donated a total of £9.3m. In 2011, for the East Africa drought appeal, 18% of UK adults donated a total of £72m. It is clear that donations to crises are disproportionately large, lending credence to the idea that there is little room for more funding in emergency aid appeals.
I still want to donate! Where should my money go?
The effectiveness of emergency aid varies massively depending on the disaster. However, out of the 5 charities involved in emergency aid that we evaluated, there are clearly some more effective places to donate: if they are active in the area, Médecins Sans Frontières (Doctors Without Borders), and if they are not, to the local Red Cross or Red Crescent society of the area where the event has taken place or the International Federation of Red Cross and Red Crescent societies. The charities on which we have focused has been guided in part by GiveWell’s prior work in this area.[11]
Médecins Sans Frontières were the most impressive emergency aid charity evaluated. They recognise that emergency aid operations are overfunded, closing appeals early[12] or even not raising any money at all for some operations.[13] To minimise response times (one of DCP2’s biggest criticisms of emergency aid), MSF has staff in 60 countries at all times.[14] They do not end an operation after only a few weeks, but only when: the situation has stabilised (e.g. in a conflict zone), or has deteriorated so much that it is now unsafe for its staff; other organisations have the capacity and motivation to restore a medical system that meets people’s needs; or the most urgent needs of victims of a disaster have been met and relief operations are no longer needed.[15] They carry out impressive evaluations of their actions. For example, one paper analysed the cost-effectiveness of two MSF surgical trauma centres: Teme Hospital, Nigeria at $172/DALY averted and La Trinité Hospital, Haiti, at $223/DALY averted.[16] They also wrote the paper on which the above case study on Haiti was based, actively critiquing their own work.
The International Red Cross and Red Crescent Movement consists of 189 National Red Cross and Red Crescent Societies run by 13 million volunteers and coordinated by the International Federation of Red Cross and Red Crescent Societies (IFRC).[17] The IFRC’s Disaster Relief Emergency Fund (DREF) is used to ensure that there is immediate financial support available for National Societies for emergency response to events.[18] The IFRC’s response to events seems very dependent on the national society: their proximity can mean excellent response times and organised relief, but they vary, and there can also be a lack of coordination or even very slow response times in some cases. Overall, the movement’s system of response and comprehensive evaluations are impressive, as is their leading role in the international humanitarian responses to disasters, although we would recommend MSF over the Red Cross/Crescent movement for larger disasters.
Conclusions
The cost-effectiveness of emergency aid in is difficult to assess: the wide range of different situations makes the effectiveness of the interventions vary massively depending on the event, and the lack of research in the area does not help the situation. But some generalisations can be drawn from the evidence we have. Emergency aid is likely to be rushed and improvised, and organisations often arrive too late to help with the short-term problems and leave too early to help with mid- to long-term problems. Lack of coordination between organisations, as well as other problems such as congestion, overcrowding and blockades are prevalent in emergency responses. These problems cannot easily be overcome with more funding, and emergency responses often receive far more than is spent, meaning that there is little room for more funding. If you still want to give, give cash not other objects, and give to charities that act more effectively with their money such as the ones mentioned here.
- Disease Control Priorities in Developing Countries, Second Edition (DCP2), The World Bank, Chapter 61, Natural Disaster Mitigation and Relief, Claude de Ville de Goyet, Ricardo Zapata Marti and Claudio Osorio, 2006,
- This section is a summary of the first two pages of "Improving Effective Surgical Delivery in Humanitarian Disasters: Lessons from Haiti" by Kathryn Chu, Christopher Stokes, Miguel Trelles, and Nathan Ford. PLOS Medicine, April 2011,
- Public health risk assessment and interventions: Earthquake, Haiti, January 2010, World Health Organization,
- Address by Mr. Cornelio Sommaruga, President of the ICRC, at the United Nations General Assembly 49th session, 23 November 1994, Accessed 23 July 2014
- Coordination of international humanitarian assistance in tsunami-affected countries, Tsunami Evaluation Coalition, Jon Bennett, WIlliam Bertrand, Clare Harkin, Stanley Smarasinghe, Hemantha Wickramatillake July 2006,
- DCP2
- CAF Disaster Monitor, A survey of the UK general public’s donations to overseas disaster appeals, Summary of trends, Liz Lipscomb, December 2011,
- UK Giving 2004/05, Results of the 2004/5 survey of individual charitable giving in the UK, Cathy Pharoah, Catherine Walker, Charities Aid Foundation; Karl Wilding, Susan Wainwright, National Council for Voluntary Organisations,
- L Lipscomb
- Ratings of Disaster relief charities one year after the Haiti earthquake | Givewell, February 2011, accessed 22 July 2014,
- Disaster relief charities | GiveWell, 2011, accessed 29 July 2014,
- Natural Disasters | MSF UK, accessed 21 July 2014,
- Japan: A note on Funding and Donations | Doctors Without Borders, March 14 2011,
- Types of Projects | MSF UK, accessed 22 July 2014,
- Closing a programme | Médecins Sans Frontières (MSF) International, accessed 23 July 2014,
- Comparative Cost-Effectiveness Analysis of Two MSF Surgical Trauma Centers, Word Journal of Surgery, Richard A. Gosselin., Andreu Maldonado, Greg Elder, 2009,
- Who we are - IFRC, accessed 22 July 2014,
- Disaster Relief Emergency Fund (DREF), accessed 22 July 2014,
Image credit: Wikipedia